Have your say on the Tech Plan for health and care
Consultation has concluded
It is important that health and care services are designed around the needs of individuals and enabled by the right technology for the best experience and outcomes.
Our Tech Plan needs to be informed and co-produced by those on the front line, who are already bringing together people, technology and infrastructure to transform health and care.
Over the next few months we will use this website to collaborate with you on the Tech Plan. We will commit to:
- Working openly
- Be clear about what can and can’t be changed
- Tell you how we have taken account of your feedback
How to get involved
We want to involve as many people as possible to help us understand how we can best support the health and care system to deliver the ambition set out in the NHS Long Term Plan and the Department of Health’s Tech Vision, as well as the forthcoming NHS People Plan.
Through this platform, you can register to participate and share your views in the following ways:
- Comment on our vision - this is a working document and will be updated as we continue to engage on this. You do not need to register to see this but you do need to register to leave a comment.
- Register or sign in to share a case study - if you want to share how you have used tech to help transform services then we would love to hear from you. You can see the contributions others have made without signing in.
Over the next few months, new ways for you to get involved in the Tech Plan will be added here. By registering for the platform, we will be able to keep you updated as we develop the Tech Plan.
If you have any queries about this work or additional comments, please send these to us at techplan@nhsx.nhs.uk
It is important that health and care services are designed around the needs of individuals and enabled by the right technology for the best experience and outcomes.
Our Tech Plan needs to be informed and co-produced by those on the front line, who are already bringing together people, technology and infrastructure to transform health and care.
Over the next few months we will use this website to collaborate with you on the Tech Plan. We will commit to:
- Working openly
- Be clear about what can and can’t be changed
- Tell you how we have taken account of your feedback
How to get involved
We want to involve as many people as possible to help us understand how we can best support the health and care system to deliver the ambition set out in the NHS Long Term Plan and the Department of Health’s Tech Vision, as well as the forthcoming NHS People Plan.
Through this platform, you can register to participate and share your views in the following ways:
- Comment on our vision - this is a working document and will be updated as we continue to engage on this. You do not need to register to see this but you do need to register to leave a comment.
- Register or sign in to share a case study - if you want to share how you have used tech to help transform services then we would love to hear from you. You can see the contributions others have made without signing in.
Over the next few months, new ways for you to get involved in the Tech Plan will be added here. By registering for the platform, we will be able to keep you updated as we develop the Tech Plan.
If you have any queries about this work or additional comments, please send these to us at techplan@nhsx.nhs.uk
Share a case study
Coronavirus (COVID-19):
As the health and care system responds to Coronavirus, we are pausing active engagement on this plan. In the meantime, you can still read the vision and mission document, and register for updates. 11/05/2020
The case studies below have been supplied by contributors and have not been checked for accuracy by NHSX.
Thank you for sharing your story with us.
Coronavirus (COVID-19): As the health and care system responds to Coronavirus, we are pausing active engagement on this plan. In the meantime, you can still read the vision and mission document, and register for updates. 11/05/2020
-
ePAQ-Pre Op
by Stephen Radley, about 6 years agoHaving developed and validated a web-based patient self-completed pre operative assessment questionnaire (ePAQ-PO), Sheffield Teaching Hospitals have implemented the technology to support a nurse-led, walk-in, one-stop Pre Op Assessment service. This was implemented in order to address escalating issues of capacity, manpower and patient flow.
Patients now go directly to a central pre-operative assessment clinic, where they self-complete ePAQ-PO using a networked PC, before seeing a nurse, who reviews their questionnaire report, arranges appropriate investigations and approves scheduling for surgery and anaesthesia.
Clinician time has been reduced by approximately 50% per patient, capacity has increased, waiting times for surgery reduced... Continue reading
Having developed and validated a web-based patient self-completed pre operative assessment questionnaire (ePAQ-PO), Sheffield Teaching Hospitals have implemented the technology to support a nurse-led, walk-in, one-stop Pre Op Assessment service. This was implemented in order to address escalating issues of capacity, manpower and patient flow.
Patients now go directly to a central pre-operative assessment clinic, where they self-complete ePAQ-PO using a networked PC, before seeing a nurse, who reviews their questionnaire report, arranges appropriate investigations and approves scheduling for surgery and anaesthesia.
Clinician time has been reduced by approximately 50% per patient, capacity has increased, waiting times for surgery reduced and patient satisfaction is high.
A prospective observational study of the impact of an electronic questionnaire (ePAQ-PO) on the duration of nurse-led pre-operative assessment and patient satisfaction https://www.ncbi.nlm.nih.gov/pubmed/30339687
The platform technology is hosted at STH, supported and provided by ePAQ Systems Ltd, an NHS spin out tech company; majority shareholder being Sheffield Teaching Hospitals NHS Foundation Trust.
-
Connected Nottinghamshire - Reducing Health Inequalities through Digital Inclusion
by Alexis F, about 6 years agoIn a rapidly evolving digital world, where digital services are becoming the default option for accessing public services, information, entertainment and each other. However many people are still facing digital, social and health inequalities because they are unable to harness the benefits that digital and online services can offer.
Connected Nottinghamshire, the digital programme across Nottingham and Nottinghamshire Integrated Care System, are starting to move towards a digital first model for health and care services in order to reduce demand, variation, over medicalisation and treatment, in order to do this as a system we recognised that we need to support... Continue reading
In a rapidly evolving digital world, where digital services are becoming the default option for accessing public services, information, entertainment and each other. However many people are still facing digital, social and health inequalities because they are unable to harness the benefits that digital and online services can offer.
Connected Nottinghamshire, the digital programme across Nottingham and Nottinghamshire Integrated Care System, are starting to move towards a digital first model for health and care services in order to reduce demand, variation, over medicalisation and treatment, in order to do this as a system we recognised that we need to support the inequalities that many of our population face.
In order to understand what issues our population faced and to target our approach in supporting them, we undertook around 18 months of research and worked with an amazing charity called The Good Things Foundation to help us understand how digital and social inclusion directly impacts health inequalities across our population and how we could help to improve this.
Utilising the digital inclusion guidance developed by Bob Gann and NHS Digital and other resources available to us we learnt that whilst overall Nottinghamshire has a low – medium likelihood of digital exclusion, those at medium – high likelihood of exclusion predominantly lived in more deprived areas, faced socio-economic challenges and were more likely to live in poverty, have lower education and housing issues. We also recognised that those people living with a long term condition, disability or illness were much more likely to be digitally or socially excluded than others.
The research that we undertook demonstrated that whilst the majority of our population did not have any barriers to accessing digital and online services over a quarter of our population did. Over 40% of those people who could not use the internet said they would like to without relying on the support of others.
The majority of the challenges and concerns which prevented people from accessing the internet were linked to concern about internet safety, not having the skills and confidence and the cost and access to the equipment to be able to do so.
So how have we addressed this?
By understanding the demographic spread of digital and social exclusion, the key socioeconomic factors and some of the issues and concerns that our population faced we developed a number of support models which could be utilised by our population across Nottingham and Nottinghamshire to reduce these inequalities.
Nottinghamshire Cancer Pathfinder
We partnered with 3rd sector organisations, charities such as Self Help UK – Beyond Diagnosis Service to see how digital could be used to improve the lives of those people living with and beyond a Cancer diagnosis. By recruiting Volunteers who already offer amazing emotional support and training them up to become a Digital Champion, they’re able to provide practical support to patients and carers from helping with online shopping or where to find up to date and trusted information.
Digital Support Hubs
Across the City and County we have established Digital Support Hubs where people can learn how to use digital devices through informal learning, having access to devices and guidance from volunteers to help improve their digital skills and confidence.
From showing someone how to get online using their smartphone or tablet, to setting up an email account and using health and care services online. Our volunteers help residents to build their confidence using the internet so they can experience for themselves the benefits it can bring to their lives.
We’ve been really keen to adopt the approach of taking health to people not the other way around, looking at the best way to engage people with digital and health – who wouldn’t normally take an interest. Alongside our static Hubs we also run a roadshow of Digital Support Pop-Up Shops.
Digital Champions Network
NHS organisations are one of the largest employers of people across the region and in order to make a significant change, we recognised that not only did we need help our population through community based initiatives, but it was vital that we supported the up skilling of our NHS workforce.
We developed a Digital Champion Network and have recruited a number of individuals passionate about championing digital services from organisations across our system. Digital Champion training was provided to 45 health professionals to date, which has improved their confidence in the use of technology so they are able to better support their peers in the development of digital skills and the population that it serves.
But we’re not stopping there; we have plans to roll the scheme out further. With 131 GP Practices across the City and County and a fantastic team of Social Prescribing – Link Workers working within our region, these front line members of staff are often asked the questions around online services by patients. By equipping our colleagues with knowledge and skills they’ll be able to better help others understand the advantages of using the internet and technology so that patients, practices and teams can benefit.
Tablet Lending Scheme
One of the main barriers to digital inclusion for some people is the cost of equipment and access to the internet. To address this, we are beginning to introduce a new scheme where iPads are available for organisations and groups across the City and County to borrow. This is so that they can discover new ways of working to help people understand the positive changes that can be made to their lives through being online, and begin to bridge the gap between adults who are offline and those online.
How Digital Inclusion is transforming lives in Nottinghamshire
Over the past 12 months Connected Nottinghamshire has supported over 600 people; ranging from supporting them in downloading, registering and navigating the NHS App to basic digital skills to support them with setting up an email, managing bills online, online shopping and information linked to hobbies; it has also recruited 45 digital champion volunteers across the NHS workforce as well as the community and voluntary sector.
The impact that this support is having on our population is significant with everyone that has interacted with the services providing positive feedback that the services has given them the confidence skills and access to support to enable them to access online and digital services on their own.
Rosie Atkin – Project Implementation Manager at Connected Nottinghamshire
Twitter - @ConnectNotts
-
Closing the Gap between Patients and Doctors: Benefits of Daily Symptom Tracking in Rheumatoid Arthritis via a Smartphone App Integrated into the Electronic Health Record
by Centre for Epidemiology Versus Arthritis, about 6 years agoThe Remote Monitoring of Rheumatoid Arthritis (REMORA) study is a smartphone study by the Centre for Epidemiology Versus Arthritis, designed to support both clinical care and research. It allows people living with rheumatoid arthritis to report daily symptoms using a smartphone app with data integrated directly into their electronic health record.
The problem: fragmented and limited data
One in four people in the UK live with a long-term condition[i]. Like in many other long-term conditions, patients with rheumatoid arthritis only see their doctor once every six months or so. Those rare visits and brief consultations fail to deliver... Continue reading
The Remote Monitoring of Rheumatoid Arthritis (REMORA) study is a smartphone study by the Centre for Epidemiology Versus Arthritis, designed to support both clinical care and research. It allows people living with rheumatoid arthritis to report daily symptoms using a smartphone app with data integrated directly into their electronic health record.
The problem: fragmented and limited data
One in four people in the UK live with a long-term condition[i]. Like in many other long-term conditions, patients with rheumatoid arthritis only see their doctor once every six months or so. Those rare visits and brief consultations fail to deliver a clear picture of patients’ symptoms and disease progression. Patients struggle to recall and summarize symptoms after such long periods of time and the short consultation does not allow them to go into much detail.
This gap between patients’ symptoms and fragmented clinical data connected to rheumatoid arthritis inspired the need of a new technology-based solution.
The solution: REMORA smartphone app
The REMORA smartphone app was co-designed with patients, clinicians and researchers to improve the collection of patient-generated health data. With daily, weekly, and monthly questions, patients consistently entered data about their health status and symptoms over a period of three months. With a simple and easy to use app patients were able to quickly score their symptoms, such as pain and fatigue, from 0 to 10. The data was then uniquely sent into their personal electronic health record – something that has not been achieved before. In parallel, it was also sent into a research database after personal identifiable information were removed. The smartphone data in the health record was then visualised in simple graphs of symptoms, allowing doctors and patients to make shared, personalised decisions.
The specific benefits of using remote monitoring of the symptoms for people living with rheumatoid arthritis included:
- providing the “bigger picture” of rheumatoid arthritis by identifying real-time changes in disease activity and capturing symptoms that would otherwise have been missed
- enabling person-centred consultations allowing doctors and patients to look together at trends of symptoms through time and make shared decisions
- empowering patients to organize and self-manage their own health
REMORA provided accessible, reusable, and reliable data that can successfully be integrated into the health records for the benefit of patients, clinicians, and researchers. Furthermore, it creates an unprecedented opportunity for the development of a patient data repository and connecting infrastructure as a blueprint for integration of patient generated data into NHS records.
A demo version of the REMORA app is available to download here.
More information on the study can be found here and in this short video. The full publication is available here.
This project was funded by Versus Arthritis and the National Institute for Health Research Collaboration for Leadership in Applied Health Research and Care (NIHR CLAHRC) Greater Manchester.
[i] Department of Health. Long Term Conditions Compendium of Information. London: Department of Health,2012. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/216528/dh_134486.pdf (2 June 2019, date last accessed). Google Scholar
-
Creating Digital Social Care Professionals - Staffordshire
by RH, about 6 years agoA small selection of social care professionals practising in Staffordshire were invited to take part in a pilot programme of digital upskilling action learning sets (ALSs) to create digital champions in social care to encourage the use of digital tools between social care professionals and their service users.
The project was undertaken to increase the uptake of Technology Enabled Care (TEC) and showcase what is possible through the introduction of digital tools and modes of delivery in front-line social care. Encouraging social care professionals to adopt and implement digital tools with service users for whom they are responsible and to... Continue reading
A small selection of social care professionals practising in Staffordshire were invited to take part in a pilot programme of digital upskilling action learning sets (ALSs) to create digital champions in social care to encourage the use of digital tools between social care professionals and their service users.
The project was undertaken to increase the uptake of Technology Enabled Care (TEC) and showcase what is possible through the introduction of digital tools and modes of delivery in front-line social care. Encouraging social care professionals to adopt and implement digital tools with service users for whom they are responsible and to make the most of opportunities for digital tools in relation to their own role, productivity and efficiency can be improved. Digital tools can help to empower service users (and their carers) to take more responsibility for their health and well-being and lead a more independent life. By enhancing engagement, focusing on prevention of deterioration of health / social conditions, technology enable care/digital tools can help to create a sustainable health and social care and provide a viable approach for more effective and productive working by social care professionals.
It is widely recognised that Information and assistive technologies can transform the way that care services are delivered but can only be an enabler if delivered appropriately to meet specific individual needs. (ADASS, 2019). In order to deliver this change the workforce must be confident, capable and competent in using modes of digital technology to improve the service provided to their users. In order to achieve interoperability and integration across health, social care and related services, front-line social care staff need to be digitally ready and confident.
Participants attended a series of three action learning sets where they were introduced to a range of digital tools intended to develop their confidence, capability and competence as local champions for technology enabled care/digital tools.
Staffordshire digital upskilling action learning programme-overview
Each individual social care professional participant was introduced to a variety of easy to access modes of technology and digital tools to assist them and their service users. Following the session each was asked to complete an action plan identifying at least two modes of technology enabled care services/digital tools they would trial within their role/with a service user. The participants ranged from those that were comfortable in using digital tools in their personal life to those that had limited experience, but all could see the value in using specific modes with their service users.
All participants were asked to complete a self-rated digital literacy questionnaire at each session – this was used to gauge their self-rated progress made between the sessions. All participants increased their use of technology enabled care/digital tools as a direct result of the programme and could see this usage increasing further if their wider social care teams adopted this approach. Many said that at the start of each service users social care journey they now had started to think where and when digital tools would be appropriate and could be used effectively for the service users well-being, whereas before participating in the course this was not a consideration. Participants could see the positive benefit of using technology enabled care and digital tools and felt confident in their ability to share this learning with their wider social care team.
At the introductory session the participants were provided with some background, explaining how an ongoing national programme for upskilling general practice nurses and clinicians had progressed and created digital champions, both in Staffordshire and also nationally, and the benefits that they had from the course, both personally and professionally and for their patients. The programme team showcased case studies of how digital tools / technology enabled care had been used in healthcare settings and advised how this could be adapted for their specific needs and be adapted for health and social care use.
All participants were asked to complete a digital literacy questionnaire at the three sessions which was used to gauge the progress throughout the course. It was positive to see that all participants increased their use of digital tools as a direct result of the programme and could see this usage increasing further as it became more embedded in their daily work life. All participants could see the positive benefit of using technology enabled care and digital tools and felt confident in their ability to share this learning with their wider team and also to other social care professionals in their area.
The results of the baseline survey show the increase in the use of digital tools/technology enabled care with service users increased during the course, at session 1, 55% of the social worker professional participants reported using digital technology for patient care 25% or less of the time but in the follow up session 88% of the social worker professionals used digital tools 50% or more of the time.
The number of social worker professionals who felt ready to use digital technology in their role increased so that by the end of the action learning programme period all felt they were ‘ready’ or ‘leading’ in relation to deploying digital technology as part of their role, compared to just 44% at session 1.
All of the social worker professionals could see the benefit of using technology enabled care/digital tools with their patients.
Modes of technology adopted
The majority of participants selected assistive technology and trusted apps to support their service users; this included those with behavioural issues, those suffering with mental health issues, and those requiring preventative and self-care interventions. Having safe and trusted apps to recommend to service users was seen as a great tool for the social care workforce, who often reportedly felt unable to adequately support their service users.
The participants could see the benefit in having a social media presence to signpost their service users to information and to share health and well-being campaigns and messages.
All of the participants were enthusiastic champions for digital delivery of care by the end of the ALS and could see how the introduction of digital tools and technology enabled care increased productivity and efficiencies.
Themes shared by Staffordshire ALS participants
The main themes emerging as outcomes of the course learning were: (1) the evolving possibilities of introducing modes of digital technology (and being aware that there is not a one size fits all approach); (2) how simple and easily accessible digital tools can have a positive impact on service users’ daily lives; (3) that digital tools can improve patient engagement/ relationships as they provide alternative modes of communication; (4) improved communications can reach a wider audience in a less intrusive way; and (5) service user empowerment – a lot of service users want to retain their independence and control, and technology can help them to achieve this.
Participants were asked what was the most important thing they had learnt from the digital champion course, with the majority answering that awareness of what modes of digital technology were available and could be utilised in their work and would make significant changes for their service users; this was a key factor in changing their perception of the worth of adoption of digital tools. A few of the participants advised that prior to the course they had no interest or confidence in the adoption of digital tools and could not really understand how this could be implemented in their line of work or be beneficial for their service users, but the ALS sessions had opened their eyes and changed their perceptions. All participants highlighted the ease of implementing digital tools in social care by using easily accessible modes of technology that are already available and readily used by service users, but just in different ways. The use of assistive technology could have a dramatic impact on a service-user’s well-being and independence and allow them to stay in their own home but be safer. The introduction of more digital tools could also be beneficial in the social care professional’s role, making aspects of their job easier and allowing them to be more efficient and effective.
-
Pioneering specialist medication automation cabinets brings efficiency and financial savings across emergency care, theatres and admission units at Northumbria Specialist Emergency Care Hospital.
about 6 years agoNorthumbria Specialist Emergency Care Hospital based in Cramlington, opened in 2015 and is the first purpose-built hospital in the country to have emergency medicine consultants on site 24/7, and specialist consultants in a broad range of conditions working seven days a week. After a successful 18-month trial of Omnicell’s systems in two North East general hospitals, a total of 24 medication automation cabinets are now in use across various departments including emergency care and theatres.
Following the success of the project, another seven medication cabinets have been installed across Northumbria Healthcare hospitals. The Omnicell systems allow clinical staff to order... Continue reading
Northumbria Specialist Emergency Care Hospital based in Cramlington, opened in 2015 and is the first purpose-built hospital in the country to have emergency medicine consultants on site 24/7, and specialist consultants in a broad range of conditions working seven days a week. After a successful 18-month trial of Omnicell’s systems in two North East general hospitals, a total of 24 medication automation cabinets are now in use across various departments including emergency care and theatres.
Following the success of the project, another seven medication cabinets have been installed across Northumbria Healthcare hospitals. The Omnicell systems allow clinical staff to order, manage and control the usage of medicines, whilst ensuring patient safety and more time for face to face patient care. The Omnicell systems are being integrated with MedChart (the hospital’s ePMA system), which is the next step in the Trust’s medicines management strategy.
The goals of implementation were to:
- Automate the ordering of medicines due to no on site pharmacy department.
- Reduce average drug spend per patient, waste and stock.
- Reduce risk of administrator errors improving safety.
- Reduce nursing, medical and pharmacy staff time spent looking for medicine cupboard keys.
- Automation of ‘top-up’ ordering, storing, rotating and organising medicines.
- Reduce inaccurate, ad-hoc ordering leading to risk of stock outs, omitted doses and treatment delays or over-stocking.
- Implement audit trail of medicines use once supplied by pharmacy.
Benefits realised since implementing Omnicell automated cabinets:
- Department nursing time savings equating to £7,000.
- Reduction in drug spend of 6% per patient.
- Stock out has fallen from 22% to 6%.
- £30,000 annual drug efficiency saving.
- Omnicell systems have improved patient care and medicines management by utilising patient safety features such as dispensing alerts for allergies, NPSA alert compliance and antibiotic stewardship.
Lauraine Gibson, Matron ED and Discharge Lounge at Northumbria Healthcare NHS Foundation Trust commented, "Without a doubt the greatest benefit has been seen in nurse time savings, with staff no longer wasting time searching for keys or medicines. These time savings which have been re-directed into front line patient care are both invaluable and rewarding for nurse and patient alike."
-
Omnicell’s automated medicines management systems are helping Leeds Teaching Hospitals to manage controlled drugs safer and faster.
about 6 years agoLeeds Teaching Hospitals is one of the biggest NHS trusts in the country. St James’ Hospital pharmacy department stock 2,500 controlled drugs and issue 2,000 controlled drug items every month. The hospital was looking for an automated system to help manage medication and controlled drugs.
The goals of implementation were to...
- Reduce clinical staff time spent preparing and dispensing medication.
- Allowing more time with patients.
- Deliver a more secure and efficient system for managing controlled drugs.
- Eliminate the written controlled drug registers.
- Deliver a full audit trail for each medication dispensed.
- Increase patient safety.
The introduction of Omnicell’s automated cabinets... Continue reading
Leeds Teaching Hospitals is one of the biggest NHS trusts in the country. St James’ Hospital pharmacy department stock 2,500 controlled drugs and issue 2,000 controlled drug items every month. The hospital was looking for an automated system to help manage medication and controlled drugs.
The goals of implementation were to...
- Reduce clinical staff time spent preparing and dispensing medication.
- Allowing more time with patients.
- Deliver a more secure and efficient system for managing controlled drugs.
- Eliminate the written controlled drug registers.
- Deliver a full audit trail for each medication dispensed.
- Increase patient safety.
The introduction of Omnicell’s automated cabinets has resulted in a number of significant benefits which include:
- Paperless process of controlled drugs from the pharmacy.
- Halved the time taken dispensing and accurately checking controlled drugs.
- Cost saving of £29k in staff time.
- Average time taken to dispense and accuracy check one stock item reduced from 6.5 minutes to 3 minutes.
- Efficiency of controlled drug management enabling compliance with the legislation, Misuse of Drugs Act and the Controlled Drugs Regulations 2013.
Deborah Armstrong, Pharmacy Patient Services Manager at Leeds Teaching Hospitals NHS Trust commented, "We are extremely pleased with our Omnicell cabinets. The implementation went smoothly and we had great support from Omnicell. Our controlled drug dispensing process is now much more efficient - we have saved 3.5 hours a day which has released staff for more patient facing activities. The average time taken to dispense and accuracy check a CD stock request has reduced from 6.5 minutes to 3 minutes! The system also provides improved audit trail and security”.
-
Electronic medication administration records improve patient safety and reduce risk of human error at The Coach House Care Home for the Elderly.
about 6 years agoThe Coach House Care Home is a 21- bed residential home for the elderly in Garforth, Leeds. The home has residents on complex medication regimes. They invested in Omnicell eMAR after becoming aware of a number of issues with their medication rounds which was then further highlighted during a CQC inspection.
The goals of implementation were to...
- Address concerns around medicines management highlighted during a CQC inspection.
- Reduce the risk of human error during medication rounds, improving residents’ safety.
- Improve the accuracy of drug counts and the time taken to do them.
- Improve the audit trail of medication rounds and... Continue reading
The Coach House Care Home is a 21- bed residential home for the elderly in Garforth, Leeds. The home has residents on complex medication regimes. They invested in Omnicell eMAR after becoming aware of a number of issues with their medication rounds which was then further highlighted during a CQC inspection.
The goals of implementation were to...
- Address concerns around medicines management highlighted during a CQC inspection.
- Reduce the risk of human error during medication rounds, improving residents’ safety.
- Improve the accuracy of drug counts and the time taken to do them.
- Improve the audit trail of medication rounds and replace a cumbersome paper-based system.
Prior to Omnicell eMAR - CQC inspection report May 2017:
- Gaps were seen in medication administration records and one person was given another person’s pain relief which was not the prescribed dosage.
- Medication audits had not identified the concerns found during the inspection.
- Medicines were not safely stored and administered.
- Notes of when medicines were not administered were not routinely recorded on the back of the MAR.
- PRN medicines were not given routinely and there was no guidance to help staff understand in which circumstances they should be offered.
- Care and treatment was not provided in a safe way for people using the service because there was no safe management of medicines.
After Omnicell eMAR was implemented - CQC inspection November 2017:
- Medicines were managed well and administration was safe. This meant the provider was now meeting legal requirements.
- There were systems in place to ensure that medicines had been stored, administered and audited appropriately.
- An automated medicines management and administration system had been introduced.
- Staff spoke positively of the new system and explained it was safer and had been introduced to reduce errors in medicines management.
- Each staff member, with responsibility for medicines, had their own sign in as an identity check and to record which staff member had administered the medicines.
- The system prompted staff if there were any safety issues involved with the medicines about to be offered.
- The system also timed the rounds to ensure people got their medicines at the correct time intervals and confirmed that all the medicines had been dispensed at the end of the round.
- People’s electronic medicine administration records included a copy of their photograph and details of any known medicines allergies to help reduce the risks associated with medicines administration.
- The eMARs showed people had received their medicines as prescribed and could also be accurately cross referenced with remaining medicines stocks to show that these were correct.
- Staff were competent giving people medicines. They explained to people what their medicines were for and ensured each person had taken them before signing the medication record.
- Staff had received training on the newly automated medicines management system. They said this training had been thorough and was supported by good back up support from the company who supplied the system. One staff member said; “It’s been brilliant, we all support each other but we also have someone we can speak to on the end of the phone. Any problems, they have been so helpful.”
Claire Buckle, Manager at Coach House Care Home commented, “The risk of human error during medication administration has been taken away since implementing Omnicell eMAR. For example, there is no longer the risk of overdosing patients as the system prompts you and tells you exactly when the resident had that last dose of medication. There has also been no incidents of missed medication errors since implementing the system. The audit trail is now much clearer as we no longer rely on a paper based system – in the event of discrepancies we can now see straight away what has happened and why it occurred. Stock counts are also much more accurate and quicker to do.”
-
Taking care of the patient data journey: success for Oxford Health NHS Foundation Trust in first step towards regional-wide interoperability.
about 6 years agoIn this case study, discover how Oxford Health NHS foundation Trust, a forward-thinking Global Digital Exemplar, embarked on a high-impact interoperability roadmap with international integration provider Enovacom that empowers NHS staff to create in-house interfaces with potential to deliver significant benefits across the health service.
Project scope
Oxford Health NHS Foundation Trust is a digitally advanced mental health, community and learning disability trust. It is a mental health Global Digital Exemplar (GDE). It provides physical, mental health and social care for people of all ages across Oxfordshire, Buckinghamshire, Swindon, Wiltshire, Bath and North East Somerset.
Services are delivered at multiple... Continue reading
In this case study, discover how Oxford Health NHS foundation Trust, a forward-thinking Global Digital Exemplar, embarked on a high-impact interoperability roadmap with international integration provider Enovacom that empowers NHS staff to create in-house interfaces with potential to deliver significant benefits across the health service.
Project scope
Oxford Health NHS Foundation Trust is a digitally advanced mental health, community and learning disability trust. It is a mental health Global Digital Exemplar (GDE). It provides physical, mental health and social care for people of all ages across Oxfordshire, Buckinghamshire, Swindon, Wiltshire, Bath and North East Somerset.
Services are delivered at multiple locations including community bases, hospitals, clinics and people’s homes. Interoperability - the ability to share and use information seamlessly across a patient journey - is vital in supporting the trust’s aim of delivering care as close to home as possible.
The interoperability challenge
Historically, interoperability has been an expensive and complicated challenge for the NHS to solve. The Five Year Forward View and its subsequent digital strategy, Personalised Health and Care 2020 set the vision for fully interoperable patient records, but Health Secretary Matt Hancock’s Tech Vision and the NHS Long Term Plan has propelled interoperability up the healthcare agenda.
The bigger picture for interoperability goes beyond integrating hospital-wide systems into developing regional shared care records through Local Health and Care Regional Exemplar (LHCRE) programmes for improving and coordinating individual care.
Oxford Health NHS Foundation Trust, facing these common integration challenges, embarked on a strategy to implement Enovacom’s user-friendly and scalable technology that will release immediate patient safety and efficiency benefits, but importantly lay the foundations for regional-wide interoperability.
The two organisations have ambitious plans to help transform healthcare on a global scale. As a Global Digital Exemplar the trust appointed Enovacom as its international partner supporting healthcare organisations across the world with learnings and best practice from their interoperability successes.
Tackling the initial challenges around interoperability
Scoping the project
Oxford Health NHS Foundation Trust prioritised three key areas for an initial proof-of-concept using the Enovacom Integration Engine.
1/ Sharing of clinical information from CareNotes electronic patient record (EPR) with external NHS organisations
Clinicians will save up to four clicks per patient case when transferring validated clinical documents and discharge summaries to GPs.
2/ Clinical information exchange from the trust’s EPR to external Child Health Information Services (CHIS)
The Enovacom Integration Engine automatically sends clinical information such as New Birth Notifications to the local CHIS removing the need for manual creations, consolidation and uploads of CVS files, saving staff time.
3/ Transferring data between CareNotes EPR and Ascribe pharmacy stock and dispensing system
The Enovacom Integration Engine will use HL7 messages to transfer data between two disparate systems: the EPR and pharmacy dispensing, and stock control system. It is arguably the biggest opportunity for immediate realisation of benefits, which are:
- Eliminating duplication of data entry - covering patient ward transfers, change in consultant or hospital discharges - on both systems
- Improving discharge process with efficient medicines management (which will follow the initial proof of concept stage)
- Patient safety, care quality and outcomes enhancements
- Reducing human error of incorrect data entry.
Early benefits around pharmacy integration
Research into potential efficiency savings from the CareNotes and Ascribe system integration through the Enovacom Integration Engine highlights positive results. The table below shows that a total of 34 hours was spent by trust staff replicating data from CareNotes to Ascribe over one calendar month. This equates to 408 staff hours and just over £9,000 in salaries annually.
Number of Admissions, transfers and discharge from Carenotes Mental Health and Community Health during November
Manual entry in Ascribe during November Number
Average Time taken to replicate 1 record in Ascribe
Total in Hours
Number of Admissions
274
2 minutes
9 hours
Number of Transfers
337
3 minutes
17 hours
Number of Discharges
250
2 minutes
8 hours
Research conducted in November 2018 has been shared courtesy of Rachel Hanks of Oxford Health NHS FT.
Data sharing for blood tests efficiency
“We discovered that we could potentially improve patient outcomes and deliver efficiencies between organisations. For example, one area we will be exploring is that if a patient is being treated by one of our clinicians here and had a blood test with another NHS organisation, we would not need to request another blood test when the result is safe enough to use. So we would save precious NHS time, effort and money from ordering an unnecessary blood test, plus the clinician has all information in front of them to make a quick analysis and outcome.” Dr Fathi Saad, EHR Systems Integration Manager, at Oxford Health NHS Foundation Trust
How will interoperability affect Oxford’s patients?
Rachel Hanks, EHR Technical Project Manager, at Oxford Health NHS Foundation Trust on delayed discharges: "Patients could get their medications quicker because staff do not have to spend their time entering information onto the pharmacy system. The faster automated data transfer reduces the likelihood of delayed discharges because medications are not being dispensed on time."
On better outcomes:
“There will be more opportunities to improve diagnosis and treatment because the information that clinicians need to make informed decisions will be available rather than having to call up other organisations to find out about a patient’s care."
Going further by partnering with Enovacom
[...]
Want to know all about this project? Download it here for free >> download
-
Medical data automation for safer and more productive care: how Wirral’s ICU nurses are benefiting from medical device integration
about 6 years agoIn this case study, discover how Wirral’s nurses are benefiting from medical device integration for a safer and more productive care, as well as how the organisation is working hard to develop workflows and blueprints for other providers to learn from their experiences around connecting mobile devices and becoming paperless.
The context:
Connecting critical data in a wired hospital
As a Global Digital Exemplar and named by the College of Healthcare Information Management Executives (CHIME) as one of the world’s ‘most wired’ hospitals, Wirral University Teaching Hospital NHS Foundation Trust prides itself on ensuring its clinical and nursing staff have... Continue reading
In this case study, discover how Wirral’s nurses are benefiting from medical device integration for a safer and more productive care, as well as how the organisation is working hard to develop workflows and blueprints for other providers to learn from their experiences around connecting mobile devices and becoming paperless.
The context:
Connecting critical data in a wired hospital
As a Global Digital Exemplar and named by the College of Healthcare Information Management Executives (CHIME) as one of the world’s ‘most wired’ hospitals, Wirral University Teaching Hospital NHS Foundation Trust prides itself on ensuring its clinical and nursing staff have access to digital tools and information that help free up time and improve care.
Connectivity between IT systems is fundamental to this ambition. The trust’s journey to HIMSS level 7 has interoperability as its heart. So, when the trust turned to Enovacom to connect highly complex data from 11 ventilators to the electronic patient record (EPR) in their busy and life-critical Intensive Care Unit (ICU), the stakes were high.
The challenge:
Delivering real-time vital signs information without compromising clinical usability
In line with national health policy, including the launch of NHSX[1], Wirral Teaching University Hospital has long recognised the value of placing clinicians at the heart of its digital strategy.
The trust empowered anaesthetists to choose ventilators that best met the clinical needs of the ITU department and Maquet ventilators were chosen. The only drawback was that the devices’ drivers would not allow connectivity and subsequent collection and transfer of patient data to the electronic patient record (EPR) real time.
“It was absolutely critical that we were confident the information was correct and that it was going into the right parts of the patient record.” Paul Young, Project Manager
Accessibility to essential data for nurses = increased patient safety benefits
Without this readily accessible data, nurses were spending excessive amounts of time double-documenting and transcribing clinical data between systems, as well as reverting to hourly manually-based methods of calculating patient’s vital signs – presenting risk of human calculation errors. The trust required a rapid and flexible solution to not only allow the exchange of critical information but also preserve the clinician’s preferred choice of medical devices.
“It is important to stress that this has been led by clinicians. The clinicians had a requirement to bring in the best clinical equipment to their department that they could use.” Paul Young, Project Manager
“It was so important we supported the nurses’ digital needs because we know that end users get disillusioned using technology that does not work for them.” Jaqui Cooper, Chief Nursing Information Officer
The specification of the biomedical interoperability project
Meeting Wirral’s requirements: automate data collection
Wirral University Teaching Hospital wanted to exchange and capture data from the new ventilators and send via the trust integration engine to the EPR system. Although this was a specific requirement to integrate two systems, the trust soon recognised the strategic benefits of adopting a flexible interoperability solution that could connect with other devices in the future, both within the organisation and across the regional Integrated Care System (ICS). As the new modern ventilators were a large investment, the trust was keen to start using them as fast as possible so clinicians would realise the benefits quickly.
“Enovacom was the obvious choice. We now have a strategic tool that meant we could stay with the clinician's preferred choice of ventilator, whilst achieving integration with the EPR - giving us the best of both worlds.” Paul Charnley, Director of IT and Information
Selecting ENOVACOM Patient Connect: a unique biomedical interoperability platform
The trust was impressed by Enovacom’s Patient Connect solution for its ability to interface with all types of medical devices, clinical applications and patient records. It offers a single interface ensuring traceability and is a 100% software-based solution supporting all clinical staff. With ENOVACOM Patient Connect, the trust would be able to integrate vital signs information via a single interface, reducing costs and resources for its IT department, whilst enhancing patient care, reducing risk and saving valuable nursing time.
The specific benefits of using Patient Connect at the trust included:
- Maintained current workflows – to avoid confusion and additional training
- Easy-to-use interface for nurses – making it is easier for them to connect data
- Enhanced mobile working – data and interfaces can be automatically monitored from mobile tablets at the bedside
- Workflows were efficient and adaptable – to meet clinical and operational requirements
“[This was] pretty much the only tool we could find that would do what we needed it to do. The depth of the product and ability to work in a flexible way to allow us to get all the granular data we needed out of the machines and in the right format to go into the EPR was one of the key things.” Paul Charnley, Director of IT and Information
Ensuring project success and clinician satisfaction
[...]
Want to know all about this project? Download it here for free >> download
[1] NHS is a government department with a mission to build digital architecture around user needs https://www.nhsx.nhs.uk
-
Personalising service for people with an urgent care need, at scale.
by Alan Kennedy, about 6 years agoThe background to the challenges regarding the delivery of effective urgent care services in the NHS are well rehearsed and include:
- Growing demand as a result of an ageing population and changes in public expectations
- Disjointed service delivery involving many different providers
- Inequitable investment in technology enabled services and a lack of community//#
system wide connectivity
- Barriers to adopting new technology enabled pathways of care
- Poor Patient experience in navigating to the right advice and definitive care
- Avoidable administrative burdens placed on clinicians
- Avoidable levels of inappropriate referrals for hospital based care etc
... Continue reading
The background to the challenges regarding the delivery of effective urgent care services in the NHS are well rehearsed and include:
- Growing demand as a result of an ageing population and changes in public expectations
- Disjointed service delivery involving many different providers
- Inequitable investment in technology enabled services and a lack of community//#
system wide connectivity
- Barriers to adopting new technology enabled pathways of care
- Poor Patient experience in navigating to the right advice and definitive care
- Avoidable administrative burdens placed on clinicians
- Avoidable levels of inappropriate referrals for hospital based care etc
In response, NHS London through the Healthy London Partnership selected the Redwood Technologies Group to develop a new Patient Relationship Management Service, to deliver more personalised services for callers to their urgent care communities. Available across the whole of the capital, Redwood overlayed their cloud based, integrated communications service called ‘ Storm’ between the national telephony provider for NHS 111 and across all of the different providers of NHS 111. This enabled London to avoid the need for a ‘rip and replace strategy’ and instead, connect legacy technologies used by local providers into a more coherent London wide solution.
Launched over four years ago through a combination of integrated communication technologies and agile programme management involving over 100 service development sprints, London has developed their Patient Relationship Manager Service to:
- Provide a London wide, real time view of provider performance across multiple urgent care systems. Including real time alerts to key members of staff in the event of an emerging problem....e.g call waiting times exceeding agreed thresholds or increases in calls related to Covid-19.
- Support development of new ways of managing demand into NHS 111. For example by using an IVR message at the front end of NHS 111 to provide an option for the caller to transfer to the local dental pain service or London wide pharmacy advice service in the event the caller has flu type symptoms.
- Support development of wholly new and personalised pathways of care using a combination of inbound call number, type of care/ crises plan and self service, as an alternative to an NHS 111 consultation. This reduces demand for 111 agents/clinicians and includes personalised pathways for people who are frail/ elderly, mentally ill/ high service user and multiple sclerosis care for example.
- Reduce the numbers of inappropriate admissions by providing NHS 111, GP Out of Hours services, Ambulance and other providers with access to multiple/ legacy/local care/ crises plans at the point of contact with 111. This included an ambulance service ‘tweet’ message sent direct to the paramedics device announcing the availability of a care plan to help support community care in the home.
- Report on syndromic demand involving d&v, flu sending real time messages to the local public health team to place a message at the front end of 111 offering local alternatives to a 111 consultation.
- Support the use of AI enabled self assessment and patient self care at the front end of the NHS 111 call, to reduce demand and support self care. This includes transfer of the data to an NHS 111 operator or clinician in the event the patient requires further support from 111. Meaning the caller does not have to repeat their history. .
- Prioritise repeat callers automatically and by transfer to the first available clinician.
More recently, the latest agile sprints within and beyond London, have focussed on testing the potential of natural language processing re:
- Taking demographic information prior to answering the call, helping to reduce call handling time/ resources.
- Supporting delivery of a greater range of self service options for callers.
- Alexa enabled self triage and onward referral to 111.
- Embedded video services using sms/web links rather than app based technologies.
- Improving compliance/assurance by using NLP based voice, data and screen recording technologies. This involves the use of technologies already deployed in mission critical command centres, airline control rooms etc and embedding it within a clinical pathway.
By way of conclusion, there are substantial benefits of using modern contact centre technologies to deliver more personalised care, especially for callers who are vulnerable or at risk of admission. One of the unique features of this NHS ‘ first of its kind’ project involved the development of a London wide communications cloud service as a separate service from technologies deployed by urgent care providers. By overlaying this commissioner led cloud over provider based legacy technologies, commissioners where able to more quickly develop and deliver changes to clinical pathways. This coupled with the use of agile change techniques effectively de risked development of these pathways.
One of the lessons learnt during this initiative is that relying on multiple provider technologies to deliver consistent and personalised care at scale, hasn’t worked. Commissioners in London, have moved beyond this and have benefitted substantially from this initiative.
Please take a look at our vision which is part of the development of our Tech Plan. You can leave comments at the bottom of this page.
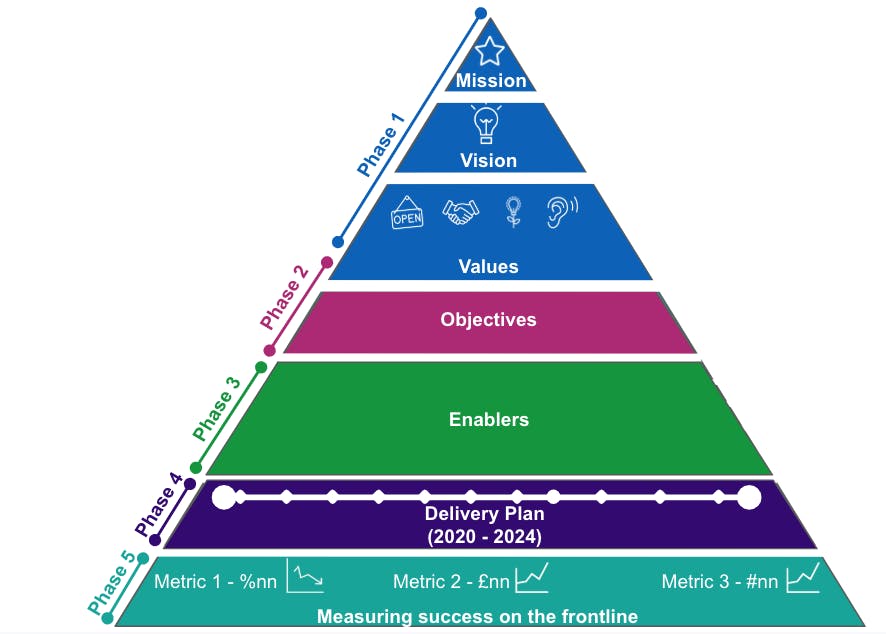
Our phases of engagement
-
Phase 1
Have your say on the Tech Plan for health and care is currently at this stageSharing our vision and starting engagement
-
Phase 2
this is an upcoming stage for Have your say on the Tech Plan for health and careOur objectives for the next five years
-
Phase 3
this is an upcoming stage for Have your say on the Tech Plan for health and careEnablers to help us realise our objectives
-
Phase 4
this is an upcoming stage for Have your say on the Tech Plan for health and careOur delivery plan
-
Phase 5
this is an upcoming stage for Have your say on the Tech Plan for health and careMeasuring success